Affordable Medicaid-Approved Therapists in NYC
How to Find and Access Therapist Services for Affordable Mental Health Care With Medicaid
Looking for Medicaid therapists in NYC? Here’s how to find one, and options available now.
Finding a therapist who accepts Medicaid can feel overwhelming, but a clear process makes accessing covered mental health care faster and more reliable. This guide defines what “therapist Medicaid services” means, explains how Medicaid mental health coverage typically works, and presents step-by-step strategies to find a Medicaid-approved therapist near you. Many people encounter barriers such as managed care networks, prior authorization, and telehealth rules; this article addresses those hurdles and shows practical verification steps to confirm a provider accepts your plan. You will learn what services are commonly covered, how copays and eligibility usually operate, condition-to-therapy mappings for common diagnoses, and the differences between telehealth and in-person therapy under Medicaid. The sections below follow an actionable path: coverage basics, search tactics, costs and eligibility, condition-specific guidance, telehealth vs in-person comparisons, and navigation resources to connect with culturally competent, trauma-informed providers.
What Mental Health Services Does Medicaid Cover for Therapy?
Medicaid typically covers a broad array of behavioral health services designed to treat common mental health conditions and support ongoing recovery. Coverage often includes individual therapy, group therapy, family therapy, crisis intervention, case management, and some longer-term community-based services, though specific limits and prior authorization rules vary by state and managed care plan. Understanding these categories helps beneficiaries know what to expect when searching for a Medicaid-approved therapist and reduces surprises at first contact. The next subsection defines common therapy modalities covered and practical examples of how they match conditions, which clarifies what to request when you contact a provider.
Which Types of Therapy Are Covered by Medicaid?
Medicaid frequently covers evidence-based therapy modalities such as cognitive behavioral therapy (CBT), dialectical behavior therapy (DBT), eye movement desensitization and reprocessing (EMDR), family therapy, and group therapy when provided by credentialed professionals. Coverage tends to focus on clinically indicated services: CBT for anxiety and depression, DBT for emotion regulation and borderline presentations, and EMDR or trauma-focused CBT for PTSD and trauma-related disorders. Some specialized modalities may require referrals or provider credentialing, and managed care plans sometimes set frequency or duration limits that trigger prior authorization. Knowing modality names and clinical matches prepares you to ask targeted questions when verifying whether a therapist who takes Medicaid can provide the treatment you need.
Before exploring telehealth rules, it helps to recognize that Medicaid programs may treat online delivery differently from in-person services, which affects how modalities are scheduled and billed.
Does Medicaid Cover Online Therapy and Telehealth Services?
Medicaid coverage for telehealth therapy has expanded significantly, and many programs now cover synchronous video and, in some cases, telephone sessions for behavioral health, though rules differ by state and plan. Telehealth parity—coverage equivalent to in-person visits—exists in many states but often includes platform, provider licensing, and documentation requirements that can affect availability for out-of-state clinicians. Privacy and HIPAA-compliant platforms, along with provider credentials, are common prerequisites; some states have made emergency telehealth expansions from recent years permanent policy while others retain stricter limits. When planning telehealth appointments, confirm technology needs, session length, and whether the therapist is listed as in-network for your specific Medicaid plan to avoid billing surprises.
How Can I Find a Medicaid Therapist or Counselor Near Me?
Finding a therapist Medicaid-enrolled in your area starts with authoritative directories and prioritized search tactics that reduce time spent calling clinics that do not accept Medicaid. Begin with your state Medicaid provider directory and managed care plan search tools, then expand to community health centers, Federally Qualified Health Centers (FQHCs), and regional behavioral health networks that list Medicaid-approved therapist options. Using targeted queries like “therapist who take Medicaid near me” and filtering by specialty (child, bilingual, trauma-informed) can surface appropriate matches quickly. And if you live in NY or NJ, you can find in-network therapists that take Medicaid here on our NYC Affirmative Psychotherapy team.
The following sections outline the best search tools and provide a verification checklist to confirm a therapist accepts your Medicaid plan before booking.
What Are the Best Ways to Search for Medicaid Mental Health Providers?
Start with the state Medicaid provider search tool or the managed care plan directory if you are enrolled in a Medicaid managed care organization—these sources list in-network therapists and clinic locations and are the most reliable for insurance acceptance. Community mental health centers and FQHCs commonly accept Medicaid and often provide sliding-scale or no-cost options for ancillary services, so include them in your search. National directories with insurance filters can help but always cross-check listings against the state directory because databases can be out of date. Prioritize providers who explicitly list Medicaid acceptance and relevant specialties (child therapy, bilingual services), then prepare to verify enrollment and network status when you contact them.
This verification step leads directly into practical phone and email scripts to confirm coverage, which can prevent scheduling delays and unexpected charges.
How to Verify If a Therapist Accepts Medicaid Insurance?
When contacting a provider, use a concise verification script: state your Medicaid plan name, ask whether the therapist is in-network for that plan, and request the provider’s NPI or billing provider name for cross-checking with your plan’s directory. Ask specific questions about copays, whether telehealth is covered under the same terms, and whether prior authorization is required for the proposed number of sessions or modality (for example, EMDR or intensive outpatient). Red flags include evasive answers about network status or requests to pay out-of-pocket without providing clear reimbursement steps; in such cases, pause and confirm with the state Medicaid help desk. Document the conversation details (date, name of staff, what was confirmed) to use if billing disputes arise later.
Confirming network status and authorization rules lets you schedule care with confidence and avoids administrative interruptions to treatment.
What Are Medicaid's Costs and Eligibility Requirements for Therapy?
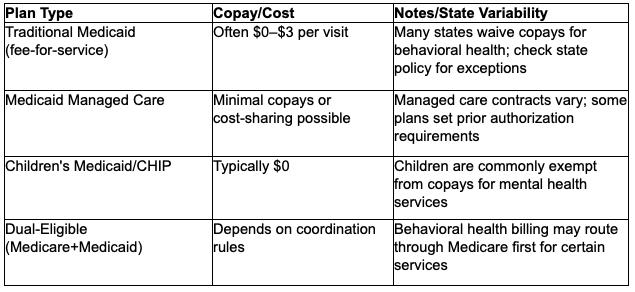
Medicaid mental health coverage generally minimizes direct costs for beneficiaries, but copays, managed care cost-sharing, and eligibility rules differ widely across states and plan types. Many Medicaid plans have low or no copays for behavioral health, and children or pregnant people are often exempt from copays, but some managed care plans can impose nominal fees or require cost-sharing under certain circumstances. Eligibility depends on income, categorical qualifications (children, pregnant people, people with disabilities), and sometimes asset tests or enrollment windows; dual-eligible seniors interact with both Medicare and Medicaid rules, which affects mental health service billing. The EAV table below summarizes typical plan types, copay expectations, and notable state variability.
Different plan types and beneficiary categories influence costs and enrollment, so the next subsection drills into common copay ranges and how to confirm exact amounts.
How Much Is the Copay for Therapy with Medicaid?
Copays for Medicaid therapy range widely: many beneficiaries pay nothing for behavioral health visits, while others may see nominal fees of a few dollars, especially under certain managed care arrangements. Exemptions are common for children, pregnant people, and in crisis or emergency behavioral health services, where access is prioritized over cost collection. To confirm, review your plan’s summary of benefits or call customer service with a provider name; asking for the exact CPT/billing code used for therapy sessions can clarify whether a visit will incur a copay. Keep records of any waivers or confirmations since state policies can change and disputes over small copays still create barriers to care.
Understanding copay norms prepares you to ask the right questions during provider verification and prevents unexpected costs from interrupting treatment.
Who Is Eligible for Medicaid Mental Health Services?
Eligibility for Medicaid mental health services generally follows program enrollment: individuals who meet income and categorical criteria—such as children, pregnant people, adults in the income bracket for expansion states, and people with disabilities—qualify for covered behavioral health services. Some states extend more comprehensive behavioral health services through waivers or state plan amendments, increasing access for specific populations like those with severe mental illness or high needs. Emergency behavioral health care is typically available regardless of routine eligibility verification, ensuring urgent access; for complex cases or appeals, contacting the state Medicaid agency or a managed care advocate can clarify pathways to covered services. If you are unsure about your status, state enrollment centers and plan customer service are the next practical contacts.
Eligibility nuances affect what services are available and how to access them, which links directly to condition-specific pathways discussed next.
Which Mental Health Conditions Are Commonly Treated with Medicaid Therapy?
Medicaid covers therapy for a wide spectrum of conditions commonly experienced by beneficiaries, including anxiety, depression, trauma-related disorders, ADHD, and substance use disorders, often within integrated care models. Treatment typically combines psychotherapy modalities appropriate to the condition, plus coordination with medication management when indicated; for example, CBT paired with primary care medication oversight for depression. Community behavioral health centers and integrated clinics provide accessible pathways for complex cases, and some programs offer specialized services like school-based therapy or trauma-informed interventions. The following sections map specific conditions to commonly covered therapies and practical service delivery notes.
How Does Medicaid Support Therapy for Anxiety and Depression?
For anxiety and depression, Medicaid commonly funds evidence-based psychotherapies such as CBT and interpersonal therapy, often delivered in outpatient clinic settings or via Medicaid telehealth therapy when available. Integrated care models that combine psychotherapy with primary care medication management are increasingly common, allowing coordinated treatment that addresses both therapy and pharmacotherapy needs. Session frequency typically follows clinical guidelines—weekly sessions initially with step-down plans as symptoms improve—but managed care prior authorization can influence intensity and duration. Recognizing these clinical pathways helps beneficiaries request appropriate services and understand how therapy and medication coordination may be billed.
Understanding treatment flow for common mood disorders prepares patients to ask about modality, expected session cadence, and how medication oversight will be arranged.
What Medicaid Benefits Exist for Trauma and ADHD Therapy?
Trauma-specific services under Medicaid often include trauma-focused CBT, EMDR, and case management supports that integrate housing, social services, and clinical care for sustained recovery, but these services can require credentialed providers and sometimes prior authorization. ADHD treatment under Medicaid typically involves behavioral therapy, parent-focused training for children, and coordination with medication management when clinically indicated; school-based services may also be a covered route for youth. Specialized interventions—such as multidisciplinary assessments or intensive outpatient programs—may require authorization or be delivered through targeted programs for high-need populations. Checking network listings for trauma-informed providers and confirming whether a therapist has specific training (TF-CBT, EMDR certification) will help you access the right level of care.
These condition-specific options emphasize the importance of targeted searches and verification when seeking specialized providers within Medicaid networks.
What Are the Differences Between Online and In-Person Medicaid Therapy?
Comparing Medicaid telehealth therapy and in-person services shows trade-offs in access, clinical suitability, and administrative requirements that affect which mode is best for a given patient. Telehealth increases geographic access, reduces travel burden, and often speeds initial appointments—advantages in provider-scarce areas and for beneficiaries with transportation or mobility challenges. In-person care can be preferred for comprehensive risk assessment, certain diagnostic testing, and hands-on interventions or when technology barriers exist. The EAV table below summarizes coverage, access, and typical pros and cons for each mode to help you decide which format best aligns with clinical needs and coverage rules.
The table below compares telehealth and in-person delivery under Medicaid, highlighting how access and coverage translate into practical benefits and limitations for beneficiaries seeking therapy. This comparison helps beneficiaries and caregivers weigh convenience against clinical needs and administrative requirements before scheduling.
| Mode | Access/Coverage | Pros & Cons |
|---|---|---|
| Telehealth (video/audio) | Widely covered in many states with provider and platform requirements | Pros: better access, flexibility; Cons: tech barriers, privacy concerns |
| Telephone-only sessions | Covered in some states under temporary/expanded rules | Pros: low tech requirement; Cons: limited clinical cues, varying coverage |
| In-person clinic visits | Standard coverage and preferred for high-acuity cases | Pros: full clinical assessment, safer for crisis; Cons: travel and scheduling barriers |
This table presents typical scenarios and considerations to guide informed decision-making for therapy modality selection.
Summary: Evaluating mode-specific trade-offs ensures you select a therapy format that matches clinical needs and coverage realities. For beneficiaries in remote areas, telehealth often provides immediate access, while in-person care remains critical for complex or high-risk scenarios. Confirm platform requirements and in-network status with providers to avoid billing surprises, and be prepared to shift modalities if clinical needs change.
What Are the Advantages of Online Therapy Covered by Medicaid?
Online therapy covered by Medicaid expands access by removing geographic barriers, offering greater scheduling flexibility and the ability to continue care during life transitions or transportation constraints. Telehealth can shorten wait times for first appointments, connect patients with specialized clinicians (such as bilingual or trauma-informed therapists) who are not locally available, and support continuity of care after hospitalization or during relocation. Technology requirements are generally limited to a smartphone or computer and internet access, though platform security and privacy standards may affect which telehealth options your plan approves. If telehealth is a fit, confirm that the therapist is listed as in-network for your specific Medicaid plan and that the platform meets any state-specific documentation or licensure rules.
Knowing telehealth advantages prepares you to ask practical questions about technology, privacy, and provider licensing during verification calls.
When Is In-Person Therapy Preferred Under Medicaid Coverage?
In-person therapy is often preferred when comprehensive risk assessments, certain psychometric testing, or close monitoring are required—circumstances common in severe mental illness, active suicidality, or complex comorbid medical conditions. Clinics also facilitate integrated services like group therapy, case management, and on-site medication management, which can be essential for coordinated care plans. Patients with technology limitations, privacy concerns at home, or those who need hands-on interventions typically receive better outcomes with in-person visits. When choosing between modes, discuss clinical indicators with a primary clinician to determine if an in-person initial assessment or periodic face-to-face sessions are necessary to meet treatment goals.
Determining modality suitability connects directly to navigating behavioral health systems and finding locally appropriate resources described next.
How to Navigate Medicaid Behavioral Health Services and Find Affordable Therapy Options?
Navigating Medicaid behavioral health services involves combining authoritative directories, local community resources, and advocacy strategies to identify affordable, culturally competent therapy options. Use state and managed care directories to find in-network therapists, contact community mental health centers and crisis lines for immediate access, and leverage case managers or social workers to coordinate referrals and benefits. Many regions offer programs that prioritize culturally and linguistically appropriate care; asking targeted questions about language services and trauma-informed training can reveal providers who meet specific cultural needs. Below we list concrete resources and explain how to evaluate cultural competency and trauma-informed practices when selecting a provider.
What Resources Help Connect Patients to Medicaid Behavioral Health Providers?
Primary resources include state Medicaid provider search tools, managed care plan directories, community mental health centers, Federally Qualified Health Centers, and regional crisis lines that facilitate urgent access and referrals. Each resource serves a role: state directories confirm network status, managed care portals provide plan-specific provider lists, and community clinics often have on-the-ground referral systems for sliding-scale services. Use a prioritized search flow—state directory first, managed care list second, then community providers—and keep detailed notes from each contact to streamline follow-up. When facing barriers, contacting a county behavioral health office or a managed care ombudsman can help resolve denials or authorization issues.
These connection tools reduce friction in accessing therapy and lead naturally to evaluating provider competence and cultural fit, discussed next.
How Does Medicaid Ensure Culturally Competent and Trauma-Informed Care?
Medicaid encourages culturally competent and trauma-informed care through provider training incentives, managed care contractual requirements, and support for language access services, producing practical indicators beneficiaries can check when choosing a therapist. Look for providers who advertise language services, cultural-linguistic competency, trauma-specific training, or experience working with specific populations such as children, LGBTQ+ clients, or older adults; these markers suggest deliberate practice toward inclusivity. Ask questions about staff training, interpreter availability, and examples of trauma-informed practices during initial verification calls to assess fit. Documenting these elements supports informed choice and helps case managers connect you with clinicians who align with cultural preferences and clinical needs.
Choosing clinicians with demonstrated cultural competence and trauma-informed approaches improves engagement and outcomes, concluding this practical navigation pathway.
State timely note: Current research and policy updates as of 06/2024 show ongoing expansion of telehealth and managed care behavioral health innovations, so verifying coverage at the point of care remains essential.
Practical next step: Use the search and verification steps outlined here to find a reliable Medicaid-approved therapist and confirm services and copays before scheduling.
If you live in NY or NJ, NYC Affirmative Psychotherapy offers Medicaid-covered online therapy for you. Click to find one of our in-network therapists that take Medicaid — we welcome all inquiries and will help match you with an affordable Medicaid-approved therapist! Get started here.
Written by Aaron Skinner-Spain, LCSW-R
Executive Director, NYCAP
Pronouns: He/Him
Education: A.B., Cornell University; M.S.W., New York University
Training: Covenant House New York-Mother and Child Program; SCO Family of Services-GLBTQ Program; SCO Family of Services East New York-High School Suspension Program; New York University Counseling and Wellness Services; Training Institute for Mental Health; Trauma Research Foundation; Parnell Institute
License: New York State #080690
Post-Graduate Training and Certifications: Executive Healthcare Leadership, Cornell University; Supervisory Training Program, Training Institute for Mental Health; Four-Year Program, Psychoanalysis, Training Institute for Mental Health; Seminar in Field Instruction (SIFI), Fordham University; Undoing Racism Workshop; The People’s Institute for Survival and Beyond
Area(s) of Expertise: college mental health, depression, anxiety, panic attacks, LGBTQ affirmative therapy, childhood trauma, acute trauma, racial trauma and stress, coping skills, AF-EMDR, clinical supervision for therapists, executive stress, and more.